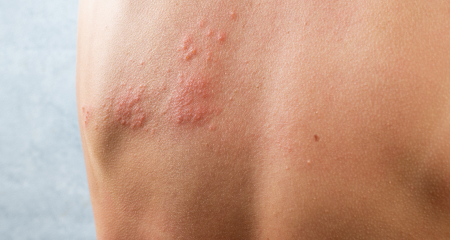
Shingles, characterized by its agonizing symptoms and localized blistering rash, often manifests unilaterally either on the face or body. While more commonly observed in individuals over 50, residents of Texas spanning all age groups are susceptible. This condition is essentially a resurgence of the dormant chickenpox virus. After an individual recovers from chickenpox during childhood, the virus doesn’t leave the system but instead hibernates in the spinal cord, only to possibly reawaken later in life as shingles.
Shingles, or herpes zoster, is a painful skin rash caused by the varicella zoster virus, which is the same virus that causes chicken pox. People who had had chicken pox, or less commonly its vaccine, are at risk of getting shingles.
Shingles occurs when the inactive form of the virus becomes active again in some of the nerves in the body. It usually occurs in people that are older than 50 and people with weakened immune systems, such as those with cancer, organ transplants, autoimmune disease and HIV. Although you can develop
shingles more than once, it is not common.
Shingles does not spread from one person to another. However, if you are in contact with someone has never had chicken pox or its vaccine, that person can develop chicken pox.
Prescription antiviral medications such as valacyclovir or acyclovir. It is best to start treatment within 72 hours of initial symptoms. This should shorten the length and severity of the rash and prevent complications including long term pain.
• If you have shingles on your face, your provider will likely send you to an eye specialist to evaluate if the virus is affecting your eye.
• The shingles vaccine is recommended for those that are high risk including anyone older than 50 and those that are immunocompromised. It is a two-dose injection that can be given at a clinician or pharmacist.
If you are concerned you have shingles, please contact our office to schedule an appointment with one of our clinicians.
