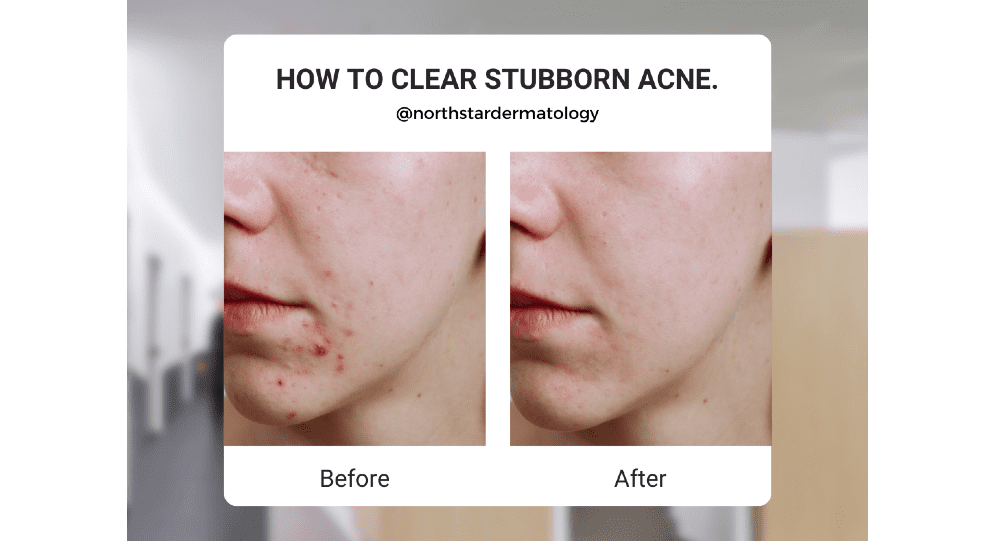
In the case of the patient pictured, there’s a strong inflammatory component, red bumps or “zits.”. To settle down the inflammation, it’ll be important to incorporate an antibacterial agent, whether topical or oral, but let’s tackle this case at its core or cause.
So what causes acne? It’s certainly NOT dirt or even dirty skin, so please stop scrubbing so hard. There are several factors at play, but the root cause is a tiny clogged pore called the microcomedone. Hormones bombard our oil glands which then pump oil, or sebum, into this clogged pore. Then, enter a bacteria called Cutibacterium acnes, which acts on this sebum to produce inflammation. This whole ensemble presents on the surface of our skin as red bumps, pus bumps, or cystic bumps. The severity of our acne has to do with our genetic background and certain environmental exposure, such as medications we take, stress, and likely the food we eat.
So if the problem is clogged pores, it would make sense that our first line of treatment would be to address the microcomedone. We do this with a retinoid product (e.g. Retin-A, tretinoin, adapalene, etc.). Many Dermatologists would argue that retinoids should have a role in every acne regimen. They’re great stuff, and not to mention, they have anti-aging and mild anti-cancer properties. Yes, there’s that eternal struggle with the redness, irritation, and peeling that come with retinoids. I typically encourage patients to try their best to power through this stage which may last 2-3 weeks. A few tricks to reducing this irritation: 1. Apply your retinoid in the early evening, and right before you go to bed, apply a nighttime moisturizer (e.g. Cerave PM) on top, 2. Dilute your retinoid by mixing it in equal parts with a moisturizer; you can also achieve this by applying moisturizer to your face first and then your retinoid on top, or 3. Apply your retinoid in the early evening, and then right before bed, wash it off and apply moisturizer. Apply your retinoid at night, because sunlight inactivates many of these products.
Also the first line in many acne regimens is benzoyl peroxide (bpo), which may come in many formulations ranging from a cleanser or a cream. Benzoyl peroxide essentially functions as an antibacterial agent, helping wipe out Cutibacterium acnes and reduce inflammation. These products also come with some drawbacks. Bpo tends to bleach linen products, so we typically recommend a cleanser that’s left on for 2-3 minutes before showering and then thoroughly washed off. Stick with lower concentrations, such as bpo 3-5%; they’re less bleaching, less irritating and just as effective. Also, some people may have allergic reactions to benzoyl peroxide. If you experience any swelling or itching after application, stop use of the product and inform your doctor.
Beyond retinoids and benzoyl peroxide, your Dermatologist may add other cleansers, topical antibiotics, or oral antibiotics to your regimen. For severe cases of scarring acne, isotretinoin (previously marketed as Accutane) is first line therapy. For “hormonal acne” occurring in women, we may add on a blood pressure medication called spironolactone. There’s an array of treatments out there and no one-size-fits-all routine. Everyone’s skin is different.
We want to briefly talk about the treatment course and expectations, as I believe patients and their Dermatologists struggle with this. We would encourage you to seek treatment early. Don’t wait until your acne is severe. Part of treatment is aimed at scar prevention, because scars are more or less permanent. Keep in mind, treatment effects are often delayed. It takes 2-3 months for most medications to start working. That is when we begin to note a difference, but you certainly won’t be clear by then, so plan accordingly if you have upcoming events. Also, treatment is an ongoing process, not an event. We start a regimen, note the effects of those treatments, make adjustments, and once clear, follow up for long term maintenance.
If you’re struggling with your acne or have questions about your skin care, reach out to a board-certified Dermatologist!