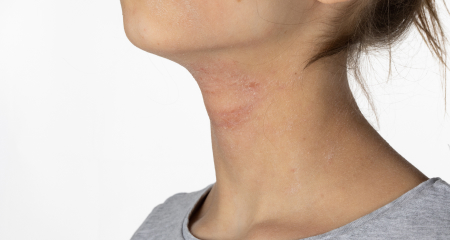
Hives, also referred to as urticaria, is a prevalent inflammation condition in Southlake, manifesting as pinkish to reddish welts on the skin. Typical symptoms encompass skin inflammation, itching, and swelling. Some individuals might notice swelling around their eyes or lips. In uncommon severe situations, there might be breathing difficulties due to the swelling of the throat. Urticaria generally arises from an overstimulated immune system, stemming from an allergic reaction or an internal issue that has a slow onset.
Urticaria, commonly known as hives, is a prevalent inflammatory skin condition characterized by pinkish to reddish welts on the skin. Swelling around the eyes or lips is also frequent, and in severe cases, swelling can occur in the throat or airways (anaphylaxis), which requires immediate emergency care. Hives result from heightened immune activity, where specific immune cells release histamine and other chemicals. While hives can be triggered by allergic reactions or external factors, in many cases, the exact cause remains unknown.
Hives are classified as either “acute urticaria” or “chronic urticaria” based on their duration. Acute urticaria generally resolves within six weeks and is often associated with allergies. Various allergens, medications, infections, and environmental factors can trigger acute hives. In contrast, chronic urticaria persists for more than six weeks. Its cause is frequently unclear, often classified as idiopathic (unknown), making this persistent form of hives challenging to manage.
The list of possible causes for hives is vast, making it occasionally tough to identify the exact trigger. And again, in over 50% of cases the cause is unknown. There are some distinct subtypes of chronic hives (chronic inducible urticaria):
• Heat urticaria
• Cold urticaria
• Cholinergic urticaria
• Solar urticaria
• Contact urticaria
• Delayed pressure urticaria
• Vibratory urticaria
• Aquagenic urticaria
The primary goal of treating hives is to alleviate itching and prevent recurrence. Keeping a journal of potential triggers can help pinpoint any specific causes, and avoiding identified culprits is crucial.
The main medical approach for hives involves oral antihistamines, often available over the counter. These include non-sedating options like loratadine (Claritin), cetirizine (Zyrtec), and fexofenadine (Allegra), as well as the more sedating diphenhydramine (Benadryl). Prescription options include hydroxyzine (Atarax) and desloratadine (Clarinex).
Topical anti-itch creams, such as over-the-counter options containing pramoxine, calamine, or menthol, can provide temporary relief. A prescription topical steroid cream, lotion, or ointment may be used, and for widespread hives, oral steroids may be given temporarily.
Managing chronic urticaria can be complex and may require exploring immunosuppressant therapy when antihistamines and topical treatments are insufficient, often with a referral to an allergist.
If hives are accompanied by swelling of the lips, mouth, or throat, difficulty swallowing or breathing, dizziness, or a racing heart, seek immediate emergency care.
