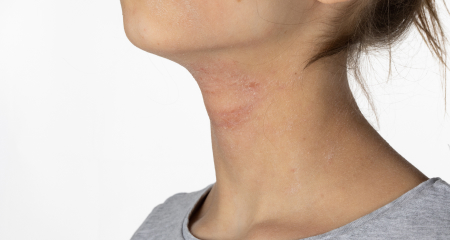
Urticaria, commonly referred to as hives, is a frequent inflammatory skin condition in Texas. It manifests as pinkish to reddish welts on the skin. Predominant symptoms encompass skin inflammation, itchiness, and swelling. Swelling around the eyes or lips is also common, and in extreme cases, there’s a risk of breathing difficulty due to airway and throat swelling. The majority of inflammatory conditions, like urticaria, stem from heightened immune system activity. Triggers could be an allergic response or a more gradual, internal imbalance.
Urticaria, commonly referred to as hives, is a common inflammatory skin condition. It manifests as pinkish to reddish welts on the skin. Swelling around the eyes or lips is also common, and in extreme cases, there can be airway and throat swelling (anaphylaxis) which requires a trip to the emergency room. Hives stem from heightened immune system activity where certain immune cells release
histamine and other chemicals. Triggers could be an allergic response or an overreaction to the external environment, but in the majority of cases the exact cause is unknown.
Hives can be classified as “acute urticaria” or “chronic urticaria” based on their duration. Acute urticaria typically resolves within six weeks and is generally linked to allergies. Numerous allergens, medications, infections, and environmental elements can cause hives. On the other hand, chronic urticaria lasts more than six weeks. Its origin is often elusive, predominantly being idiopathic (i.e., unknown), and this
persistent form of hives can be difficult to treat.
The list of possible causes for hives is vast, making it occasionally tough to identify the exact trigger. And again, in over 50% of cases the cause is unknown. There are some distinct subtypes of chronic hives (chronic inducible urticaria):
• Heat urticaria
• Cold urticaria
• Cholinergic urticaria
• Solar urticaria
• Contact urticaria
• Delayed pressure urticaria
• Vibratory urticaria
• Aquagenic urticaria
The main goal of treatment is to reduce itching and prevent hives from recurring. Keeping a record or diary of potential triggers can help identify any potential cause, and if there are any culprits then avoidance is key.
The main medical treatment for hives is oral antihistamines, which are usually over-the-counter and include non-sedating (non-sleepy) options such as loratadine (Claritin), cetirizine (Zyrtec), and fexofenadine (Allegra), and the more sedating diphenhydramine (Benadryl). There are prescription options such as hydroyxyzine (Atarax) and desloratadine (Clarinex).
Topical anti-itch creams can temporarily reduce symptoms and include over-the-counter lotions containing pramoxine, calamine, or menthol. A topical steroid cream/ lotion/ ointment can be prescribed. Oral steroids may be given temporarily if the hives are extensive.
Managing chronic urticaria is often intricate with varied success. In cases where topical treatments and antihistamines prove insufficient, immunosuppressant therapy might be explored to mitigate the excessive immune reaction, and may require referral to an allergist.
Remember, if hives develop along with symptoms of swelling of the lips or inside the mouth or throat, problems swallowing or breathing, feeling lightheaded or faint, or racing heart, this warrants emergency
care with prompt attention at an emergency room.